For two decades, the conversation about hormone replacement therapy has been shaped by safety concerns that have steadily eroded prescribing confidence. A new Danish nationwide cohort study, published in The BMJ in February 2026, offers the largest real-world reassurance yet.
Researchers at Copenhagen University Hospital followed every Danish woman born between 1950 and 1977 who was alive at her 45th birthday. That gave them a cohort of 876,805 women, tracked through national prescription and mortality registries for a median of 14.3 years. Of these, 104,086 (11.9%) filled at least one prescription for systemic menopausal hormone therapy.

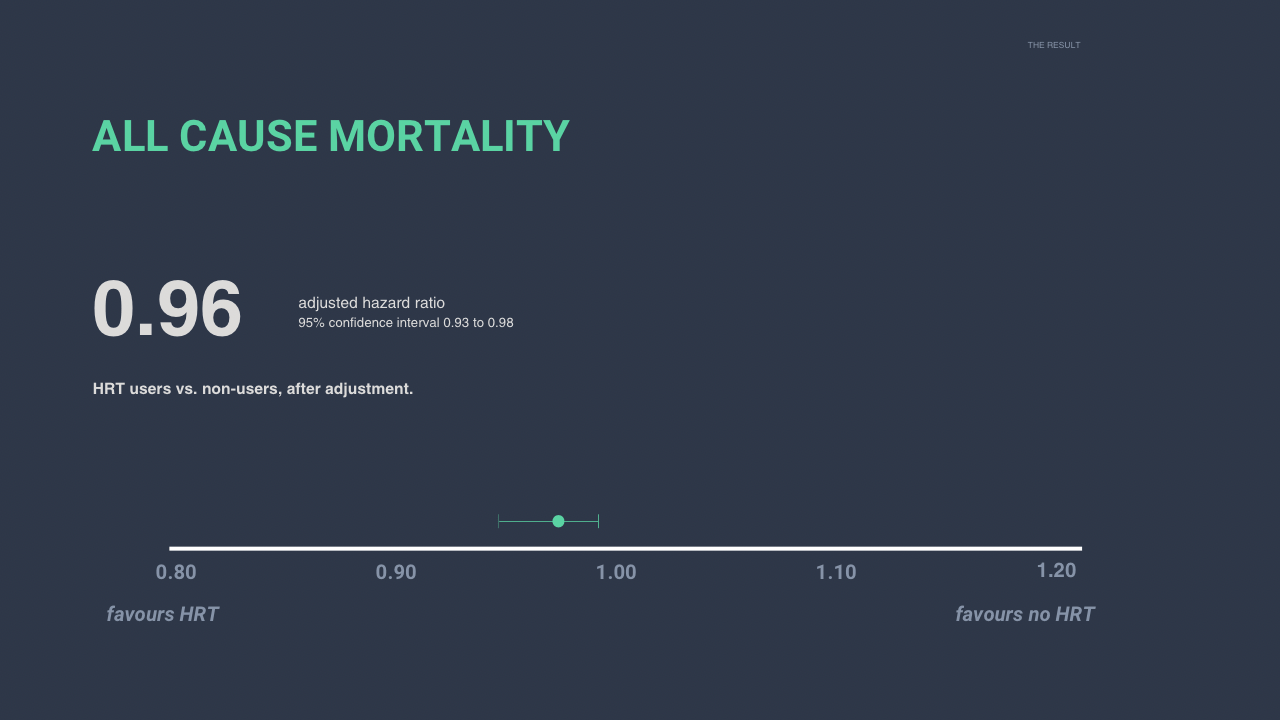
After adjustment for age, parity, education, income, country of origin, and comorbidities including diabetes, hypertension and cardiovascular disease, the adjusted hazard ratio for all-cause mortality among HRT users was 0.96 (95% CI 0.93 to 0.98).¹ In other words, no signal of excess mortality.
The cause-specific analyses tell the same story. There were no robust differences in deaths attributed to cardiovascular disease, stroke, or cancers of the breast, womb, or ovary.¹ Long-term users (those on therapy for ten years or more) showed no excess risk either, addressing one of the most persistent clinical anxieties around cumulative exposure.
One subgroup finding stood out. Women who underwent bilateral oophorectomy between ages 45 and 54 for non-cancerous reasons had meaningfully lower mortality when using HRT, prompting the authors to suggest more women in this group might benefit from being offered it.
The caveats matter. This is observational data, and the authors acknowledge residual confounding cannot be excluded. Healthy user bias is plausible: women prescribed HRT may differ in unmeasured ways from those who are not, including smoking and BMI, neither of which were captured. Women with prior thrombosis, liver disease or hormone-sensitive cancers were excluded, so the findings cannot be extended to higher-risk groups.

For UK primary care, this sits alongside the updated British Menopause Society practice standards, which already recommend against arbitrary limits on HRT duration, dose or age. The Danish data add population-level mortality evidence to a guideline position previously built largely on symptom and quality-of-life outcomes.
Reference
Mikkelsen AP, Bergholt T, Lidegaard Ø, Scheller NM. Menopausal hormone therapy and long term mortality: nationwide, register based cohort study. BMJ. 2026;392:e085998. doi:10.1136/bmj-2025-085998
Medicine Central is a clinical evidence review for UK primary care clinicians. Content reflects evidence current at time of publication and should be read alongside local formulary and clinical guidance. For healthcare professionals only.
